Submitted by: Chloe Powell, Johnson Ma, Nicole Dorfan
Highlights
ACT Teams provide therapeutic mental health and substance use assessments and interventions.
────
Our data supports the integration of clinical psychologists into ACT teams to enhance capacity and provide equitable services.
────
Policy makers and healthcare administrators can include psychologists into ACT teams as a first step to addressing barriers to accessing mental health care.
Since the 1970s, mental health care has evolved to become increasingly recovery-oriented in Canada. To transform to the changing landscape, literature has called for Assertive Community Treatment (ACT) teams to improve clinicians’ training and implementation of evidence-based practices. Clinical psychologists possess in-depth training and unique skills valuable in supporting ACT programs transforming to a recovery-oriented framework (Bronfenbrenner, 1979).
Between 2015 and 2016, the British Columbia Coroners service reported that there had been a 140% increase in deaths of people experiencing homelessness with most of these individuals dying between the age of 40–59 years (BC Coroners Service, 2019). The complexity of risk factors for early mortality in these individuals is a subset of multimorbid factors that represent the coexistence and overlap of serious physical, mental, cognitive, and substance use conditions (Vickery et al., 2021). An individual experiencing homelessness costs the Canadian government approximately $55,000 per year in health and corrections services (BC Non-Profit Housing Association, 2020).
“We’re missing Yoda, we’re missing the Jedi Master, we don’t have that guidance and supervision . . . I think I would probably cry if we got a psychologist on our team. . .just having that knowledge base at the end of the phone that is dedicated to us and our questions and our clients. We could go from helping people exist and stay out of hospital to actually thriving.”
Given both the increased risk of mortality and economic burden, it is necessary for interventions, such as ACT, to be optimized to address homelessness and the social determinants of health. In recent years, ACT has been criticized as “paternalistic” and “coercive” (Van Veen et al., 2018) yet the current findings indicate that ACT has made commendable efforts toward integrating recovery-oriented and person-centered interventions.
How Did A Community Psychology Perspective Inform Your Work?
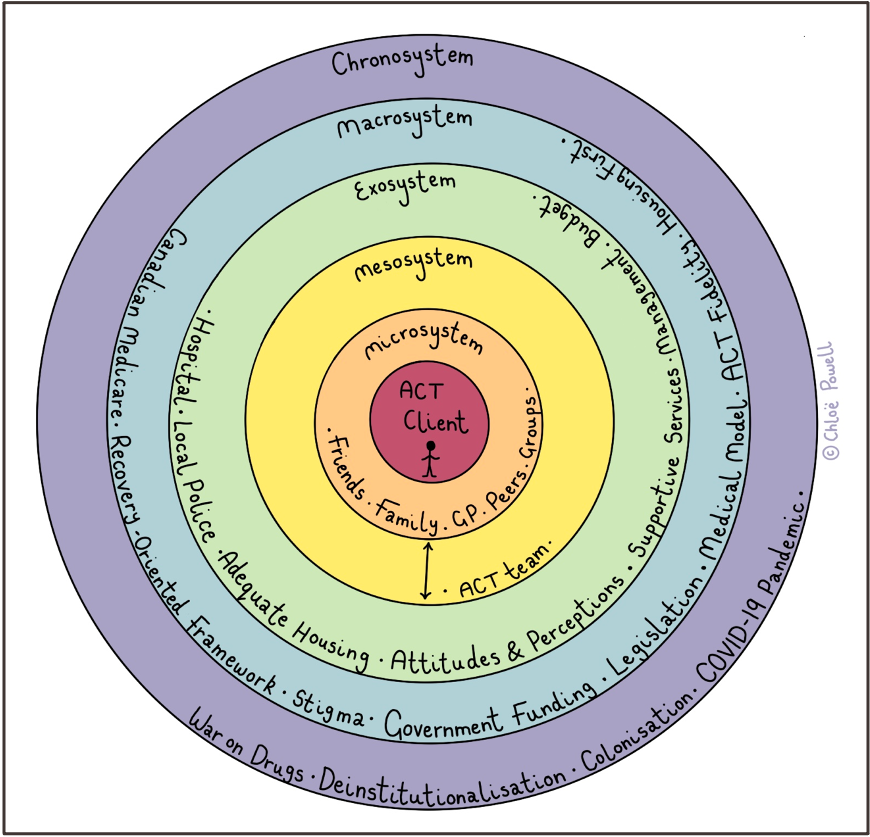
Community Psychology emphasizes the need to consider the intersection of local, national, cultural, and political contexts when conceptualizing human distress. With Bronfenbrenner’s ecological systems model in mind, interventions cannot just focus on the individual (i.e., the individual client serviced by the ACT team or the individual ACT team). To address the systemic barriers identified by the project, investment is needed in strategies and interventions such as, increased funding to ACT programs, improved access to adequate and affordable housing, and public campaigns to shift attitudes and perceptions of mental health.
Methods
Semi-structured interviews were conducted with 10 participants (including social workers, occupational therapists, recreational therapists) employed on 9 ACT teams in both British Columbia and Ontario. Thematic analysis revealed that shared beliefs and perspectives were held by the participants (ACT practitioners) in the study, despite being employed on different ACT teams across Canada.
Results
- ACT practitioners utilize multimodal interventions (i.e., both evidence-based and informal therapeutic interventions) within a recovery-oriented framework. However, evidence-based interventions are utilized on an “ad-hoc” basis due to barriers including, clients’ level of wellness, lack of clinical guidance, and limitations in training.
- ACT practitioners unanimously supported the inclusion of clinical psychologists into ACT programs, particularly in terms of improving access to supportive services (e.g., comprehensive assessments, psychotherapy), providing training opportunities (e.g., in evidence-based interventions, case conceptualization), and providing clinical supervision and/or consultation.
- ACT practitioners emphasized that psychologists would need to be flexible in their approach (e.g., willing to conduct outreach) to meet the unique demands of the ACT program and client population.
- ACT teams continue to face significant systemic barriers including budget constraints, limited housing opportunities, safety issues, staffing issues, and burnout.
What Does This Mean For?
Research and Evaluation: Our team only recruited participants who were employed on the ACT team. Future research may want to explore perspectives of ACT clients regarding their experience of ACT and provide an opportunity to voice any concerns, advocate for their needs, and individualize their care.
Practice: The project provides initial data supporting the integration of clinical psychologists into ACT programs. Next steps could be a pilot program in which clinical psychologists are integrated into ACT teams on a trial period.
Social Action: Integrating clinical psychologists into ACT teams could be the first step in improving the representation of clinical psychologists in public and community mental health settings. Moreover, currently, clinical psychologists are not included in the Canadian public health care plan. The inclusion of clinical psychologists into ACT programs could be an immediate, initial step to integrating psychological services into Canada’s publicly financed healthcare system. Doing so could improve equitable access to mental health care by reducing excessive wait-times, accessing hard-to-reach populations, and reducing the burden on other health professionals (e.g., family physicians, community mental health teams).
Similar Settings: Many doctoral-level training efforts have a limited focus upon community mental health, which could impact their level of preparedness for working in this field. There are no existing dual-track or single-track doctoral-level community psychology programs in Canada. More dual-track community and clinical psychology programs should be developed, and social justice/community psychology frameworks should be integrated into all applied psychology training institutions, coursework, and practica.
To learn more, connect with C. Powell on Instagram @bepsychminded
References
BC Coroners Service. (2019). Reportable deaths of homelessness, 2007 – 2016. https://www2.gov.bc.ca/assets/gov/birth-adoption-death-marriage-and-divorce/deaths/coroners-service/statistical/homeless.pdf accessed 8.2.2023
BC Non-Profit Housing Association. (2020). 2020 homeless count in Metro Vancouver. https://www.vancitycommunityfoundation.ca/sites/default/files/uploads/HC2020_FinalReport.pdf accessed 9.27.2023
Bronfenbrenner, U. (1979). The ecology of human development: Experiments by nature and design. Harvard University Press.
Van Veen, C., Ibrahim, M., & Morrow, M. (2018). Dangerous discourses: Masculinity, coercion, and psychiatry. In J. M Kilty & E. Dej (Eds.), Containing madness (pp. 241–265). Palgrave Macmillan. https://doi.org/10.1007/978-3-319-89749-3_11
Vickery, K. D., Winkelman, T. N., Ford, B. R., Busch, A., Robertshaw, D., Pittman, B., & Gelberg, L. (2021). Trends in trimorbidity among adults experiencing homelessness in Minnesota, 2000-2018. Medical Care, 59(Suppl 2), S220–S227. https://doi.org/10.1097/MLR.0000000000001435 accessed 9.27.2023
Original Citation: Granski, M., Javdani, S., Anderson, V. R., & Caires, R. (2020). A Meta‐Analysis of Program Characteristics for Youth with Disruptive Behavior Problems: The Moderating Role of Program Format and Youth Gender. American Journal of Community Psychology, 65(1-2), 201-222. accessed 9.27.2023